
Performing physical examinations is becoming a lost skill, but Brian Garibaldi, MD, is on a mission to turn that trend around.
A few trends and events have set the stage for the decline of these skills. For starters, there is no standardized curriculum to teach physical exam skills in graduate medical education. The assumption is that these skills are taught in medical school, so residents already know how to do them by the time they enter residency. “The problem is students learn the basic techniques in the first and second year of medical school without the context of understanding disease, so they don’t really understand how these techniques can serve them in making a diagnosis,” noted the ABMS Visiting Scholar from the Class of 2017–2018. Increasingly fewer practicing physicians are able to accurately teach these skills to trainees. There are also few standardized tools to assess trainees. Direct observation often falls short because it does not routinely occur and when it does, it’s qualitative and subjective, said Dr. Garibaldi, who is the Associate Program Director of the Osler Internal Medicine Residency Program at The Johns Hopkins Hospital. Residents don’t see other physicians modeling physical exam skills in the hospital. Instead, they spend 60 percent of their time in front of a computer, gleaning information from the electronic medical record (EMR).
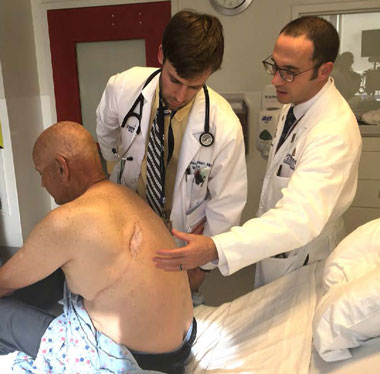
To preserve physical exam skills, Dr. Garibaldi and his colleagues created the Assessment of Physical Exam and Communication Skills (APECS), adapted from the MRCP – Practical Assessment of Clinical Examination Skills (MRCP-PACES). In a pilot study, which was the focus of his Visiting Scholars’ research project*, this tool was used to assess 72 internal medicine interns from The Johns Hopkins Hospital who rotated through a cardiovascular, pulmonary, and neurology station examining a patient and presenting their findings to faculty. They were assessed in exam technique, identification of physical signs, differential diagnosis, clinical judgment, and maintaining patient welfare. Faculty provided 10 minutes of real-time feedback and bedside teaching. Scores were compared between the interns who rotated through the skills curriculum and those who did not. The pilot study demonstrated the feasibility of using a PACES-style assessment for U.S. trainees. Inter-rater reliability was high, suggesting that this methodology is a valid way to assess physical exam performance, he noted. Both trainees and patients appreciated the direct feedback and education given by the faculty preceptors.
While the goal was to educate residents, an unexpected benefit is that the faculty also learned. “We are very intentional about pairing junior faculty with more senior or experienced clinicians,” Dr. Garibaldi said. “So not only are we teaching the residents skills, but the faculty learn from each other. By the end of the day, everybody is better.”
The pilot has since been expanded thanks to a grant from the Center of Innovative Medicine at Johns Hopkins. It now includes five physical exam stations where residents encounter eight patients, seven of whom are actual patients with real findings on both physical exam and history. Faculty has expanded as well. This year alone, 40 faculty members have become preceptors, adding to the 10 existing preceptors from the pilot. Every internal medicine intern from The Johns Hopkins Hospital and Johns Hopkins Bayview Medical Center rotates through the curriculum; 73 of 74 interns across both campuses participated in 2019. The original program focused on cardiac and pulmonary disease because 30 percent to 40 percent of hospital patients have related health issues, Dr. Garibaldi explained. The expanded program includes gastroenterology. It also incorporates bedside point-of-care technology, such as ultrasound, because of its growing role in real-time diagnosis.
This year, the program will be expanding to Stanford University and University of Alabama at Birmingham as part of a $1.8 million grant awarded to the three institutions by the American Medical Association (AMA) last month. The grant will be used over the next five years as part of the AMA’s Reimagining Residency Initiative designed to study the impact of the training environment on physician burnout among internal medicine residents. Approximately four years ago, physician educators at the three institutions collaborated to reinvigorate bedside training, which eventually lead them to form the Society of Bedside Medicine, a nonprofit organization dedicated to bedside teaching and improving physical exam and diagnostic skills.
With the additional data and further study, Dr. Garibaldi believes that the APECS assessment tool can answer the question, “Does improved bedside physical exam skill lead to tangible outcomes?” He and his colleagues will evaluate test utilization, cost of care, and behavior in the hospital, that is, how much time the residents spend at the bedside versus on the EMR, as part of the AMA initiative. Today’s physicians spend more time with the EMR than they do at the bedside, he said. But if they improve their physical exam skills would they spend more time at the bedside and less time on the EMR? “One hypothesis about physician burnout is that when you spend all the time in front of a computer, you find less meaning in the work you are doing,” he said. If physicians spent less time on the EMR would they experience less burnout? Would that change in behavior lead to improved patient outcomes? After all, the physical exam is fundamental to accurate diagnosis and patient-centered care that begins at the bedside.
Dr. Garibaldi also has thought about the tool’s potential as a continuing certification activity. Given the combination of assessment and learning that occurs with the use of APECS, he would like to see if it’s possible for faculty to earn continuing certification credit for participating in the program.
Dr. Garibaldi is hopeful that this work will inspire other physicians to recognize the value of the physical exam, help physicians improve their skills to perform them, and train a cadre of faculty to teach them. Seems like it already has.
Learn more about the ABMS Visiting Scholars Program and who should apply.
* Dr. Garibaldi’s project was supported by a grant to the ABMS’ Research and Education Foundation from the Gordon & Betty Moore Foundation.
© 2019, American Board of Medical Specialties.
